Lipoprotein(a): Genetic Cholesterol Risk and What You Can Do About It
Feb, 27 2026
Most people know about LDL cholesterol - the "bad" kind that clogs arteries. But there’s another silent player in heart disease that doesn’t show up on routine blood tests: lipoprotein(a), or Lp(a). It’s not just another number on a lab report. For about one in five people worldwide, Lp(a) is the reason their heart disease came out of nowhere - even if they eat well, exercise, and don’t smoke. And here’s the kicker: you can’t fix it with diet or pills. It’s written in your genes.
What Exactly Is Lipoprotein(a)?
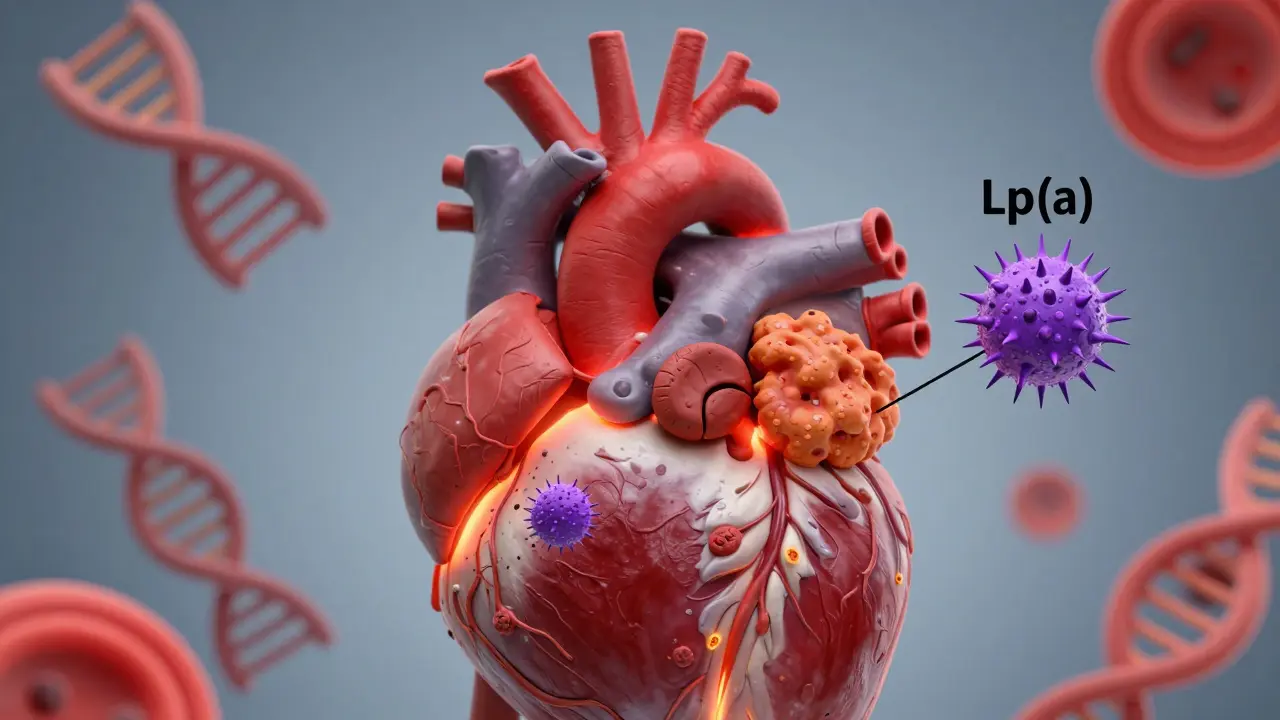
Lp(a) is a weird hybrid. Think of it like an LDL particle - the kind that drops cholesterol into artery walls - but with a strange extra protein glued on: apolipoprotein(a). That extra piece doesn’t just sit there. It sticks to damaged areas in your arteries, grabs onto blood clots, and stops your body from breaking them down. The result? Plaques grow faster. Clots stick longer. Your risk of heart attack, stroke, and even aortic valve narrowing goes up - no matter how healthy you are otherwise.
It was first spotted in 1963 by a Swedish scientist named Kare Berg. Back then, no one knew what to do with it. Today, we know Lp(a) is one of the most powerful inherited risk factors for heart disease - more than high blood pressure, more than diabetes, more than obesity. And it’s not rare. About 20% of people globally have levels high enough to raise their risk. Yet, most doctors never test for it.
Why Most People Never Know They Have High Lp(a)
Standard cholesterol panels? They don’t measure Lp(a). Not even close. You need a specific blood test - and your doctor has to request it. That’s why so many people find out too late. A 42-year-old woman with no family history of heart disease, normal LDL, and a clean lifestyle has a heart attack. Her doctor runs more tests. Her Lp(a) is 180 mg/dL. That’s like having the same risk as someone with familial hypercholesterolemia - a known genetic monster of cholesterol.
Here’s the hard truth: if you’re not tested, you’re flying blind. The American Heart Association says levels above 50 mg/dL (or 105 nmol/L) are a red flag. Above 90 mg/dL? That’s severe risk. Some people have levels over 300 mg/dL. That’s not just high - it’s a ticking time bomb.
And here’s another surprise: Lp(a) levels barely change over your lifetime. Unlike triglycerides or LDL, they don’t spike after a fatty meal or drop with exercise. They’re set by your genes - and stay that way. That’s why screening early matters. If you’re over 40 and have no idea what your Lp(a) is, you might be missing a major clue.
Your Genes Are the Main Driver - Here’s How
More than 90% of your Lp(a) level comes from your DNA. Specifically, from a gene called LPA. This gene controls how many "kringle IV" repeats are in the apolipoprotein(a) protein. More repeats? Lower Lp(a). Fewer repeats? Higher Lp(a). It’s one of the strongest genetic links to disease in the entire human genome.
That means if one parent has high Lp(a), you have a 50% chance of inheriting it. It’s that simple. No lifestyle choices, no luck. Just genetics. And it doesn’t skip generations. If your grandparent had a heart attack at 50 and no one knew why, Lp(a) might be the hidden cause.
Some populations are hit harder. Black individuals, on average, have Lp(a) levels 2-3 times higher than white, Hispanic, or Asian groups. Women often see a rise after menopause - estrogen normally holds Lp(a) down, and when it drops, Lp(a) climbs. That’s why a 55-year-old woman with no other risk factors might suddenly need to worry.
What High Lp(a) Actually Does to Your Body
Lp(a) doesn’t just raise cholesterol. It attacks your arteries in three ways:
- Builds plaque: Like LDL, it drops cholesterol into artery walls - but it does it more aggressively.
- Sticks to clots: The kringle domains latch onto fibrin (the mesh that forms clots), making them harder to dissolve.
- Blocks cleanup: It interferes with plasmin, your body’s natural clot-busting enzyme. So clots last longer - and grow bigger.
The result? Higher risk of:
- Heart attack
- Stroke
- Peripheral artery disease (poor circulation in legs)
- Aortic valve stenosis (narrowing of the heart’s main valve)
Studies show that people with Lp(a) above 125 nmol/L (about 50 mg/dL) have a 2-3 times higher risk of heart attack. And if you already have heart disease? High Lp(a) makes your next event more likely - and more severe.
Why Statins Don’t Help - and What Does
Here’s where most people get confused. If you have high Lp(a), your doctor might put you on a statin. But statins? They barely touch Lp(a). In fact, some studies show they might even nudge it up a little. That’s because statins target LDL production - not the LPA gene.
Niacin (vitamin B3) can lower Lp(a) by 20-30%. Sounds good - until you remember the side effects: flushing, liver damage, high blood sugar. Most people can’t tolerate it long-term. And even if it lowers Lp(a), we still don’t know if that translates to fewer heart attacks.
So what’s the real hope? A new class of drugs called antisense oligonucleotides (ASOs). One drug, pelacarsen, has shown up to 80% reduction in Lp(a) in early trials. It works by silencing the LPA gene - literally telling your liver to stop making the bad protein. The big phase 3 trial - called Lp(a) HORIZON - is tracking over 10,000 people with very high Lp(a) and existing heart disease. Results are expected in 2025. If it works, this could be the first treatment ever proven to prevent heart events by targeting Lp(a) directly.

What You Can Do Right Now
Even if you can’t lower Lp(a) yet, you can still lower your overall risk. Think of it like this: Lp(a) is the fuel. Everything else - smoking, high blood pressure, diabetes - is the spark. You can’t change the fuel, but you can remove the sparks.
- Lower your LDL: Keep it under 70 mg/dL if you have high Lp(a). Statins help here - and ezetimibe or PCSK9 inhibitors may be needed.
- Control blood pressure: Aim for under 120/80. High pressure damages arteries - and Lp(a) loves to stick there.
- Don’t smoke: Smoking doubles your risk. Period.
- Manage diabetes: If you have it, keep your HbA1c under 7%.
- Stay active: Even if it doesn’t lower Lp(a), exercise reduces inflammation and improves blood flow.
- Eat smart: Focus on whole foods, fiber, omega-3s. Avoid trans fats and excess sugar.
And if you have a family history of early heart disease (before age 55 for men, 65 for women), ask your doctor for an Lp(a) test. Don’t wait for a heart attack to happen.
Who Should Get Tested?
You should consider an Lp(a) test if:
- You’ve had a heart attack, stroke, or peripheral artery disease before age 55 (men) or 65 (women)
- You have a family history of early heart disease or sudden cardiac death
- You’ve been diagnosed with familial hypercholesterolemia
- You have high LDL despite treatment
- You’re Black or have a family background from populations with known higher Lp(a)
Testing is simple: just a single blood draw. No fasting needed. The test is called "Lp(a) by immunoassay" - and it must be specifically requested. Don’t assume it’s done.
What’s Coming Next?
By 2025, we may have the first drug approved specifically to lower Lp(a) and prevent heart events. That’s huge. But even before then, labs and guidelines are improving. The American College of Cardiology now recommends universal screening for adults at least once in a lifetime. That’s a shift from "test only if suspicious" to "test everyone."
Scientists are also digging into whether hormones, liver disease, or kidney function affect Lp(a) levels. So far, evidence is weak - but if we find triggers, we might find new ways to manage it.
For now, awareness is the best tool. If you’ve been told your cholesterol is "fine" but still worry about heart disease - ask. Get tested. Knowledge isn’t just power. It’s prevention.
Is lipoprotein(a) the same as LDL cholesterol?
No. Lp(a) is a separate particle that includes an LDL-like core but has an extra protein called apolipoprotein(a) attached. While LDL delivers cholesterol to artery walls, Lp(a) does that too - but it also promotes clotting and blocks clot breakdown. Standard cholesterol tests don’t measure Lp(a), so you need a specific blood test to find out your level.
Can diet and exercise lower lipoprotein(a)?
Not significantly. Unlike LDL or triglycerides, Lp(a) levels are mostly fixed by genetics - over 90% determined by your LPA gene. While healthy eating and exercise help reduce overall heart risk, they won’t meaningfully lower Lp(a). That’s why doctors focus on controlling other risk factors like blood pressure, smoking, and LDL cholesterol when Lp(a) is high.
How do I know if I have high lipoprotein(a)?
You need a specific blood test. Standard lipid panels don’t include Lp(a). Ask your doctor for an "Lp(a) test" - it’s not automatic. Levels above 50 mg/dL (or 105 nmol/L) are considered high risk. If you have a family history of early heart disease, or if you’ve had a heart event before age 55/65, testing is strongly recommended.
Is lipoprotein(a) more dangerous than other cholesterol types?
For some people, yes. Lp(a) is an independent risk factor - meaning it adds risk even if your LDL and HDL are normal. People with very high Lp(a) (above 90 mg/dL) have a risk level similar to those with familial hypercholesterolemia. It’s also more heritable than hypertension or diabetes. But it’s not "worse" for everyone - it’s just a hidden risk that many doctors overlook.
Will new drugs cure high lipoprotein(a)?
Not a cure - but potentially a major breakthrough. A new drug called pelacarsen, an antisense oligonucleotide, has shown it can lower Lp(a) by up to 80% in clinical trials. The phase 3 trial (Lp(a) HORIZON) is testing whether this reduces heart attacks and strokes. Results are expected in 2025. If successful, this will be the first treatment proven to target Lp(a) directly and reduce cardiovascular events.
If you’ve been told your heart health is fine but still feel uneasy - ask for the Lp(a) test. It’s not a luxury. For one in five people, it’s the missing piece.
